The telehealth trend, accelerated by COVID-19, is not limited to Maine. But the state is becoming an attractive market for for telehealth developers like Senscio Systems. The state’s health care providers are embracing the trend, too.
Get Instant Access to This Article
Subscribe to Mainebiz and get immediate access to all of our subscriber-only content and much more.
- Critical Maine business news updated daily.
- Immediate access to all subscriber-only content on our website.
- Bi-weekly print or digital editions of our award-winning publication.
- Special bonus issues like the Mainebiz Book of Lists.
- Exclusive ticket prize draws for our in-person events.
[bypass-paywall-buynow-link link_text="Click here to purchase a paywall bypass link for this article"].
Home has been lonely during the pandemic for 73-year-old Portland resident Mary Gagnon, but a bit less so thanks to regular check-ins with a virtual medical care team through a touch-screen tablet and phone calls.
“It’s easy to use, and the fact that you’re being observed without any intrusion I think is great,” she says of the device that helps her manage chronic conditions including heart trouble, diabetes, COPD, arthritis and fibryomyalgia.
Multiple times a day, she’s asked how she feels and about her breathing, and gets reminders about when to take her temperature, use an oximeter to measure blood-oxygen levels and when to take different medications.
“It’s good to have someone keeping an eye on me so my children don’t have to do it every day,” says Gagnon, who lives in Avesta Housing’s subsidized Butler School building in the city’s West End. “Somebody else does it.”
Gagnon is among more than 60 Avesta Housing residents — most of whom are seniors or disabled — using a tablet provided free of charge by Senscio Systems, a Boxborough, Mass.-based telehealth solutions developer, in partnership with Avesta.
Senscio’s Ibis service, which would cost uninsured members between $125 and $225 a month, includes a 10-inch tablet to report daily symptoms, medical equipment to monitor temperature and other vitals, a dedicated Ibis physician to create a care plan and routinely review health data. Users are also assigned a member advocate to connect them with community resources, and care is coordinated with their primary care doctors and specialists.

Like many of her neighbors, Gagnon is a convert to technology — and using it for medical care — during the pandemic. Besides the tablet, she’s been using Zoom to talk with her doctors even though “I don’t like anything complicated.” Virtual telemedicine medicine visits have spiked during COVID-19 and become popular with older adults.
Even before that, Maine’s profile as the nation’s oldest state was an attraction for Senscio Systems, along with having the largest proportion of people eligible for both Medicare and Medicaid, according to co-founder and CEO Piali De.
The India-born, Ivy League-educated physicist and inventor founded the Senscio Systems in 2010 with her husband, Hugh A. Stoddart, and late father-in-law, Hugh F. Stoddart, whose illness informed much of what they built. Today the company employs about 30 people. That includes eight in Maine, where it opened an operations center in Scarborough just before COVID. It plans to hire more than 500 in the next three years.

Though the company has been in the telehealth business for five years, De says the pandemic has turned it into a “hot field” that’s here to stay. In Senscio’s case, it’s not just a matter of providing artificial intelligence-powered smart devices and remote services. It is also gathering and using data to change patient behavior — including by catching problems a human doctor might not — as well as to improve care for specific populations.
“We’re telehealth with a capital T,” she says of Senscio, whose pilot program with Avesta was launched in 2019 and really took off during the pandemic.
Senscio is active in three states, with more than 650 people so far — including those currently being enrolled — using the Ibis program and technology to manage chronic conditions. They’ve used the system to complete more than 3 million self-management tasks.
“When we started our business,” De says, “we saw that this continuous chronic health care management is something that does not exist in our health care system.” While the current, fundamentally episodic health care system is premised on doctors seeing patients only when there’s a problem, “our premise is that we’re going to keep an eye on you when nothing’s wrong.”
Fixing what it sees as a broken chronic system is yielding both medical and monetary benefits for members, in terms of better health outcomes and lower medical costs. That’s reflected in a 70% reduction in hospitalizations, a 36% reduction in long-term nursing care and as much as a fourfold increase in the length of time between hospitalizations.
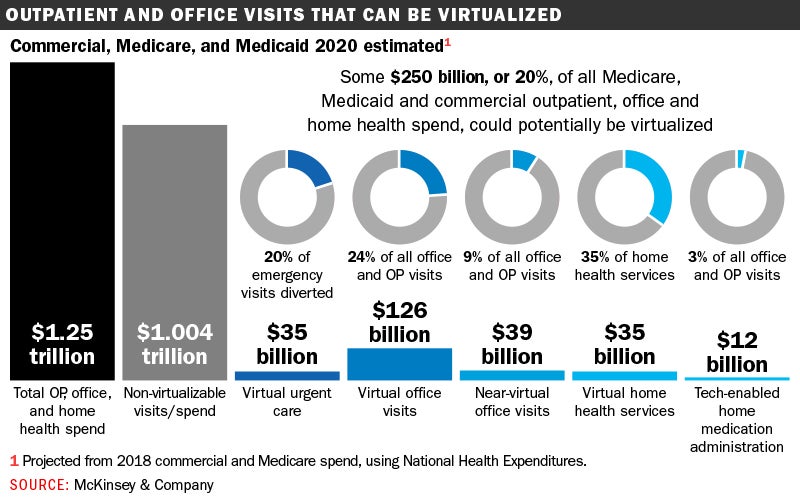
Potential to the tune of $250B
The telemedicine trend, accelerated by COVID-19, is not limited to Maine, as reflected in data from the federal Centers for Medicare and Medicaid Services. After an average 13,000 telehealth visits a week by Medicare beneficiaries before the public health emergency, that number was up to 1.7 million by the end of April. It cites early data showing telehealth to be an effective way for people to access health care safely during the pandemic, whether to get a prescription filled, manage chronic conditions or get mental health counseling.
A report by consulting group McKinsey & Co. published in May shows a similar trend for the broader population. It found that the percentage of U.S. consumers using telehealth has climbed from 11% in 2019 to 46% when the report came out, with providers reporting 50 to 175 times the number of telehealth visits than pre-COVID.
Looking ahead, McKinsey analysts estimate that up to $250 billion of current U.S. health care spending could potentially be done virtually, including close to a quarter of all office visits or outpatient services and 20% of emergency department visits. They also note that the shift will not be inevitable and point to a gap between consumer interest and actual usage, driven in part by a lack of awareness of virtual offerings and understanding of insurance coverage.
Closer to home, Massachusetts-based nonprofit benefits provider Harvard Pilgrim Health Care reports a dramatic jump in telehealth usage in the four New England states it serves since February, including a 6,817% increase in Maine.
Harvard Pilgrim’s Bill Whitmore, vice president for the Maine market, says that while the percentage of general office visits by Harvard Pilgrim members via telehealth have gone down from 70% during the summer peak to around 40% now, the percentage of behavioral health visits has stayed around 80%.
“If people are more willing to have a behavioral-type visit via telehealth, then maintaining that capacity is critical,” he says. But he also points to barriers, including the lack of broadband access in rural areas and the large number of independent and small physicians’ offices that may not have the resources to deliver those services like video and computer equipment.
“It’s not a huge investment, Whitmore says, “but any investment for some of these small practices is not necessarily easy.”
While regulation often lags technology, it’s moved relatively quickly at state and federal levels during the pandemic with regards to telehealth. Measures include an executive order from Gov. Janet Mills that allows licensed medical professionals greater leeway in providing telehealth services and an order by Eric Cioppa, the state superintendent of insurance, that aligns Maine with federal guidance on insurance coverage and makes telehealth more affordable.
On the national front, the federal CARES Act aid package passed in March has eased restrictions on telehealth during COVID-19, helping make the service widely available.
“This was a critical step, which helped ensure that patients can access their healthcare providers without taking on extra risk,” says U.S. Sen. Angus King, I-Maine. “These policies made a difference, and there’s no reason they have to end when the pandemic does.”
Even as medical practices reopen and in-person visits pick up, he’s confident telehealth is here to stay.
“This is anything but a fad,” King tells Mainebiz. “It’s a real shift in the way that Americans access health care with enormous benefits for Maine patients and businesses. We should make sure it continues beyond this crisis.”
Health providers seeing a surge
Providers seeing a surge in virtual visits during the pandemic include ConvenientMD Urgent Care, a Portsmouth-based company with clinics in New Hampshire, Massachusetts and Maine, where it has five locations.
It has recorded about 40,000 virtual visits since mid-April, averaging about 280 a day, with six out of 10 visits from outside the catchment areas of its clinics.
“It’s been the busiest time in the history of our business,” says Mark Pundt, CovenientMD’s president and chief medical officer.
“We were already contemplating the use of telehealth before the pandemic, and realizing that medicine in some ways would follow the retail industry, where malls and big-box stores are losing ground to Amazon,” he says. “For medicine, it would be going from large hospital big boxes to virtual forms of care.”

ConvenientMD plans to keep investing in technology to expand telehealth while building further bricks and mortar sites, including in Ellsworth. Originally scheduled to be ready in 2020, that’s now been moved to March 2021.
“We stepped back on all development until we knew where COVID was headed, but the volume at all of our clinics across the three states is higher than planned,” he says. “We’re performing better than we had prior to COVID.”
Maine-based health care systems MaineHealth and Northern Light Health are equally committed to expanding their telehealth capabilities after the pandemic-fueled spike in demand.
MaineHealth, the largest health care system in New England and Maine’s largest private employer, has used telehealth going back to 2000 and ramped that up during the pandemic. That will continue with several federally funded projects, including a $1.15 million project to buy equipment for hospital telehealth and to serve at-risk, rural populations.
Jasmine Bishop, MaineHealth’s director of telehealth, says the team is growing as MaineHealth considers vendors including Senscio Systems to build out its remote patient monitoring program and analyzes qualitative data from telehealth patient surveys to see where any adjustments may be needed.
“It’s an iterative process, and both patients and providers have been so understanding of any glitches,” she says. “We have the opportunity to reduce the potential for those as we move into a new world” when fear of the coronavirus subsides. “It’s really going to test how well-adapted telehealth will be.”
At Northern Light Health in Brewer, Matt Weed, the chief strategy officer, sees telehealth as a key component of the customer service mix for patients. He was one himself in May, seeing an orthopedic surgeon virtually at Northern Light Eastern Maine Medical Center for a sore shoulder.
“We had face-to-face contact, the surgeon had a good camera and was able to see that I had a good range of motion,” Weed says. “I really got everything I could have gotten from an in-person visit, though if surgery had been indicated that would have required an in-person visit.” That was not the case, he says, “and everything was done beautifully through telehealth.”
‘As much as we want it to be’
Back at Avesta Housing, resident services manager Nick Kjeldgaard is pleased with how the partnership with Senscio Systems is going and the Ibis tablets’s growing popularity with elderly residents.
“I would suggest that most people who are using them now continue to use them once things are back to normal,” he says. He’s equally excited about the prospect of using the data to see where Avesta can improve care for residents, like through classes on balance or nutrition.
“This can be as much as we want it to be,” he says.
