Emergency treatments: Trying times for Maine’s rural hospitals spark entrepreneurial approaches
 Photo / Jim Neuger
Marie Vienneau leads two rural hospitals in Maine including Northern Light Mayo Hospital in Dover-Foxcroft, shown here.
Photo / Jim Neuger
Marie Vienneau leads two rural hospitals in Maine including Northern Light Mayo Hospital in Dover-Foxcroft, shown here.
More Information
As head of operations for LifeFlight of Maine, Bill Cyr has a front-row view of the turbulence at hospitals across the state’s small towns and villages.
“The rural places are really rural,” says Cyr, a former flight nurse who’s been in health care since high school. Today at LifeFlight, he oversees operations for the Bangor-based nonprofit serving 136 communities, islands and unorganized townships from bases in Bangor, Sanford and Lewiston with three helicopters, a fixed-wing airplane and a growing fleet of ambulances.
During the pandemic, hospitals treated critical patients for longer, secured ventilators and other life-saving equipment and trained staff quickly on new skills, Cyr says. Today, “they do the best that they can with what they have, and they figure it out.”
With about half of America’s rural hospitals operating in the red, there’s a lot to figure out in order to tackle staffing shortages, reduced reimbursements and lower margins.
In Maine, the country’s oldest state with a median age close to 45, rural hospitals care for some of the state’s sickest, poorest and oldest residents. Many live in sparsely populated areas with subpar internet connectivity and transportation hurdles.
Michael Topchik, an analyst with Chartis Group LLC, a Chicago-based health care consultancy, points to the erosion of a rural health safety net developed after World War II to bridge the divide between urban, wealthier areas and less-populated agrarian regions.
He also says that rural hospitals are being paid less for their services while grappling with ever-changing reimbursement models, particularly around Medicare Advantage plans.
“Programs and safeguards that were put in place have eroded. Reimbursements have eroded,” says Topchik, who is based in Portland.
“There’s an old saying, ‘No margin, no mission,’ and every one of these rural hospitals has a mission to support their local community and their health care needs. It’s pretty tough to do that if you can’t keep the lights on.”
Widening national crisis
While America’s rural health safety net has been in crisis for 15 years, the situation has gotten worse over the past year, according to a report by Chartis published in February.
Over the past year alone, the percentage of rural hospitals operating in the red jumped from 43% to 50%, the single-largest change in a 12-month period. The situation is leading to “care deserts” in rural areas, with many dropping services from obstetrics to inpatient care and more than 500 facilities nationwide considered vulnerable to closure.
The downsizing comes as hospitals are no longer able to rely on government programs that sustained them during the pandemic.
In addition, growing enrollment in Medicare Advantage — a health plan offered by Medicare-approved private insurers — is eating into the bottom line for the very entities the federal “critical access hospital” designation was meant to buttress when it was created in 1997.
Medicare Advantage, for example, may not cover all the services traditional Medicare does, and prior authorizations can lead to increased denials, according to Chartis.
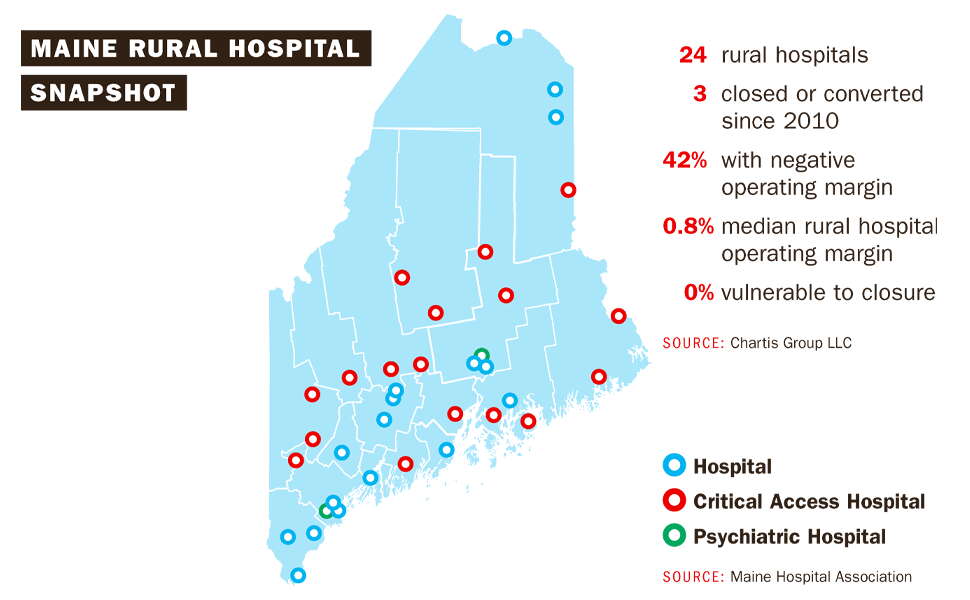
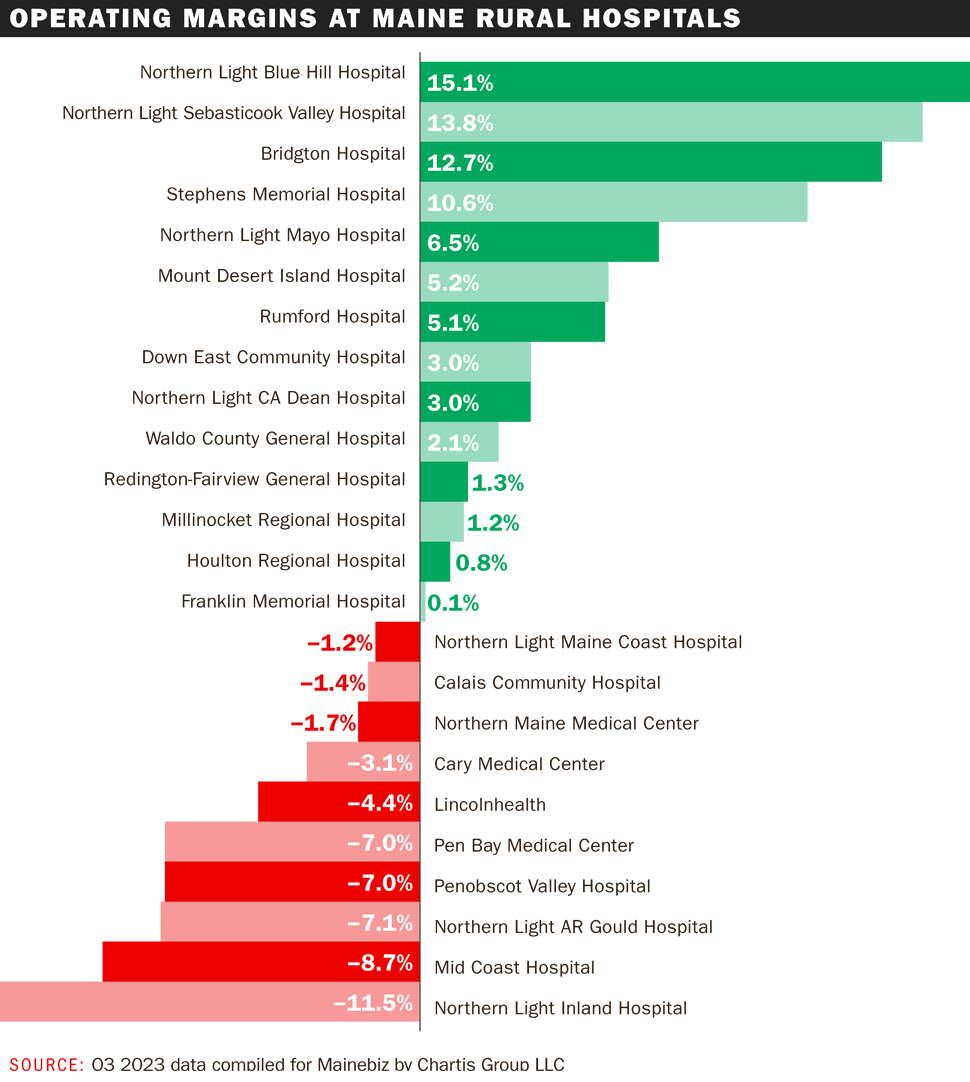
Today in Maine, 24 of the state’s 38 hospitals are in rural areas, home to an estimated 40% of the population in 11 counties. Out of those 24, 10 had negative operating margins in the third quarter of 2023, according to data compiled for Mainebiz by Chartis. That adds up to an average operating margin for all 24 at 0.8%, or just above break-even.
“It’s not a great time for hospitals in general, and it’s even more difficult for rural hospitals, especially those that are not within a system,” says Marie Vienneau, president of Northern Light Mayo Hospital, a 25-bed critical access hospital in Dover-Foxcroft, and the 15-bed Northern Light CA Dean Hospital in Greenville, both of which had third-quarter 2023 operating margins on the plus side, according to Chartis.

‘Innovating to survive’
Forced out of necessity to become more resourceful, some of Maine’s smaller hospitals are finding ways to invest in upgrades and even expansions. Many are also tackling the shortage of doctors and nurses with new approaches to recruiting and training, whether in-house, with outside help or in collaboration with their peers.
“Rural hospitals are innovating and investing in order to survive and provide the best care to their patients,” says Steven Michaud, president of the Maine Hospital Association. “Infrastructure decays whether we like it or not, and it is imperative for the hospitals to invest wherever they can. It also allows them to improve patient safety, service and access to care.”
In Farmington, Franklin Memorial Hospital is in the process of changing from a fixed-rate Medicare and Medicaid reimbursement model to a cost-based one as a recognized critical access hospital.
The locally controlled nonprofit integrated network of rural health care providers, created by Franklin Memorial Hospital in 1991, has been part of the MaineHealth system since 2014.
To change its designation, the hospital has downsized from 65 patient beds to 25, still enough to cope with the patient numbers of recent years. Congress created the CAH designation in 1997 in response to over 400 rural hospital closures during the 1980s and early 1990s. The law has been tweaked over the years, most recently with a broader definition of the required distance between facilities.
The main reason for Franklin’s conversion is to get higher reimbursements.
“Commercial payers pay us about 50 to 60 cents on the dollar over actual cost, or about 150% to 160% — sometimes a little more, sometimes a little less, depending on the contract negotiation — for what we bill,” says Barbara Sergio, FCHN’s president.
“And then your government payers — Medicare, MaineCare and Medicaid — will typically pay 30 to 40 cents less than cost on the dollar, or about 60% to 70%, if you’re a regular hospital. When you convert to a critical access hospital, it’s 101%. It’s cost-based reimbursement — whatever it costs to run our rural hospital is what they reimburse us.”
That difference is huge “because we can’t survive on 30 to 40 cents less than cost on the dollar,” she says. “A lot of hospitals, whether they’re large or small, if they’re in urban areas, if you have a strong commercial payer, it can make up the difference. But when you live up here in rural Franklin County, we just don’t have that. We don’t have enough to keep us afloat.”
Indeed, the hospital had a 0.1% operating margin in the third quarter of 2023, Chartis data show.
With financial backing from MaineHealth, Franklin is in the process of an $11 million emergency-department upgrade and a $4 million expansion of oncology and infusion.
Too small to have its own doctor residency program, FCHN participates with other regional institutions in the state-funded Maine Rural Graduate Medical Education Collaborative, abbreviated as MERGE. The hospital also plans to participate in a federally funded MaineHealth rural residency program to be launched in 2027.
“In building new opportunities for teaching residents here in Maine we could not go it alone,” says Dr. Ross Isacke, an internist at Franklin Memorial and FCHN’s chief medical officer who has worked in both rural and urban settings.
“A lot of people don’t think they could practice rurally, but when they see what it’s like to live and practice in a rural setting, it’s a lot less daunting,” he says.
Upgrades in Piscataquis County
In-house training is also a priority at Northern Light Mayo Hospital in Dover-Foxcroft, a 4,550-population town in Piscataquis County.
One example is a nursing program at the hospital in collaboration with Eastern Maine Community College that’s hosted two cohorts to date. Out of 10 graduates so far, seven are still working at Mayo.
However, without enough graduates from Maine nursing programs to fill staffing shortages, the hospital continues to employ travel nurses, who are three times more expensive.
“Our goal is to have 100% of our own employed nurses. We make progress every week on that, but that will take a while,” says Vienneau, whose childhood admiration for Florence Nightingale inspired her own career in nursing.
“I always said I was going to be a nurse when I was a little kid, but I never said I was going to be a health care administrator,” she says outside the leafy grounds of Mayo, which recently reconfigured its emergency department. “You don’t have to look far to see you’re making a difference in the community when you’re in a very small place like this.”
About 45 minutes away in the 1,530-population town of Greenville, she also leads Northern Light CA Dean. It’s Maine’s smallest hospital with just 15 beds in a brand-new $27 million building with new equipment from a CT scanner to modern lab analyzers — a far cry from the equipment that hospitals used to share back and forth in Vienneau’s nursing days.
“In rural areas, you have to be extremely creative in how you provide the service so that people in your community can have access,” she says, highlighting the entrepreneurial nature of running a rural hospital. “You have to be not afraid to try new things.”

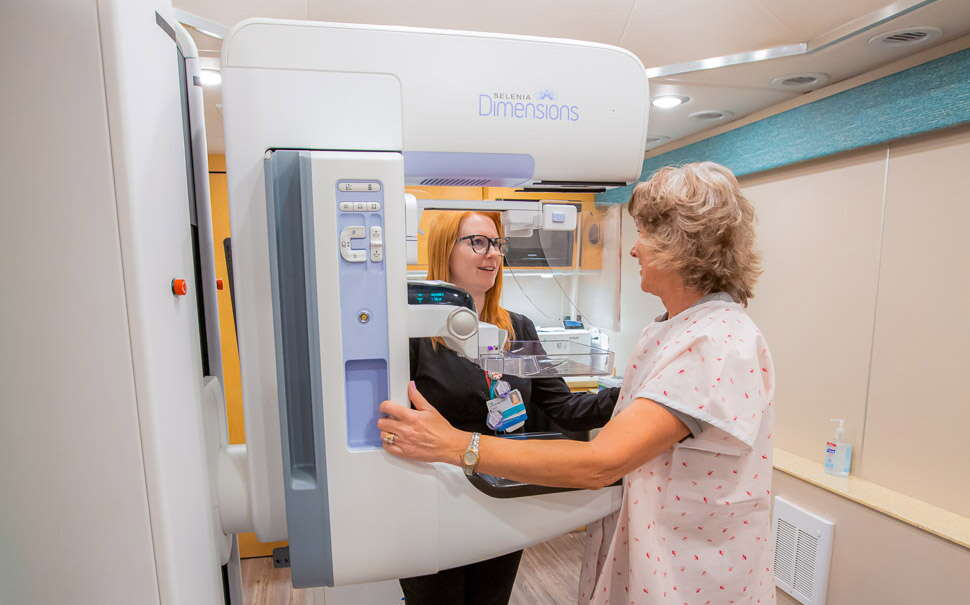
Another innovation at CA Dean Hospital is a mobile mammography unit purchased with more than $1 million in congressionally directed funds and supported by a $160,000 Maine Cancer Foundation grant to employ a women’s health advocate to identify patients who are due or overdue for screenings, get them scheduled and arrange transportation if needed.
The mobile unit is outfitted with the same 3D technology used in hospitals to produce high-quality images and aims to mirror what patients would find in any hospital-based mammography setting. The unit, based in Greenville but also often in Monson, has screened 100 patients so far.
Next month, the aim is to start going to the Jackman Community Health Center, which is owned by Penobscot Community Health Care, and other communities after that.
“Only two-thirds of women in Piscataquis County over the age of 40 have had a mammogram in the past two years, and per capita breast cancer deaths in the region exceed the state and national averages,” Vienneau says. “Given the rural nature of our communities, having a mobile unit is key — more women in more places will get screened.”
Staffing up in Waterville
In Waterville, Northern Light Inland Hospital is a 48-bed community hospital with primary and specialty care physician offices in Waterville, Oakland, Unity and Madison, as well as a continuing care facility on the Waterville campus.
Tackling staffing issues like the rest of its peers, Inland recently worked with a Texas-based staffing company to bring on three orthopedic surgeons to provide 24/7 coverage in Waterville.
“We had been recruiting orthopedic surgeons for over three years with no luck, but when we partnered with them, we had full coverage within four months,” Tricia Costigan, the hospital’s president, says. Impressed with the arrangement, she says her hospital is assessing how other services are staffed and whether it makes sense to expand scheduling flexibility for other providers.
“We haven’t come up with concrete solutions, but we’re definitely trying to use this new model to see if there’s a way to be creative in other specialties,” Costigan says.
Elsewhere on the staffing front, Inland works with institutions including Portland’s Northern Light Mercy Hospital, which dispatches two of its cardiologists to Waterville twice a week.
“Together with many community partners, we are working to address and support multiple initiatives for our region,” Costigan says. Inland also recently added a surgical robot that’s being used by obstetrician-gynecologists and general surgeons, and is “actively recruiting other minimally invasive surgical specialties needed by our community,” she notes.
Describing health care as a “science-based career that’s led with your heart,” Costigan says that “whether or not a community thrives is tied to two things — their schools and their health care. There’s something to be said for neighbors caring for neighbors.”
Editor's note: Article updated to add clarification about payments from Barbara Sergio.














0 Comments