Hospitals in transition: Maine's hospitals face challenges to their own well-being
It's hard to keep up with the changing landscape of Maine's 37 hospitals. Consider that just in the month of August:
• Maine Coast Memorial Hospital in Ellsworth signed a letter of intent to begin the process of joining Eastern Maine Healthcare Systems in Brewer, which, if an agreement is reached, would make the 64-bed facility the ninth hospital in the EMHS system.
• Franklin Community Health Network became the 30th member of the MaineHealth system after getting an OK from the state.
• Mercy Hospital submitted “conceptual plans” to the city of Portland for a consolidation of services at an expanded Fore River Parkway campus that would include an ambulatory care center and the closure of its downtown hospital.
The Jan. 1 merger of Southern Maine Medical Center and Goodall Hospital, creating Southern Maine Health Care, resulted in combined staffs and operations along with a new board of directors, and a decision by Pen Bay Medical Center and Waldo County General Hospital to share a CEO and some services in order to cut costs.
Add to the mix the Affordable Care Act, the continuing debate on expanding Maine's Medicaid program and the loss of revenue resulting from proactive health care initiatives designed to keep people healthy and out of the hospital.
To put all this in context, Mainebiz asked Steven Michaud, who's been president of the Maine Hospital Association since 1999, to share with our readers the perspective of Maine's 37 hospitals that collectively employ 30,000 people and, in many cases, happen to be the largest employers in their region. The following is an edited transcript of our interview.
Mainebiz: How would you describe these times in general for Maine's hospitals?
Steven Michaud: I've been with Maine Hospital Association for 27 years and I've never seen anything like it. It is the most tumultuous time for hospitals that I've ever seen. The Affordable Care Act is just part of it. Another fundamental issue is that federal and state governments are broke and that means that there's extraordinary pressure on Medicare and Medicaid, which are our biggest payers. There also has been an unprecedented explosion in uncompensated care, free care. Part of the reason we've got so much uncompensated care is that if you've got a $2,000 deductible, let's say, and you're of modest means, you're not always able to pay that $2,000 if you've got a major procedure. So a lot of that gets swallowed as 'bad debt' by Maine hospitals.
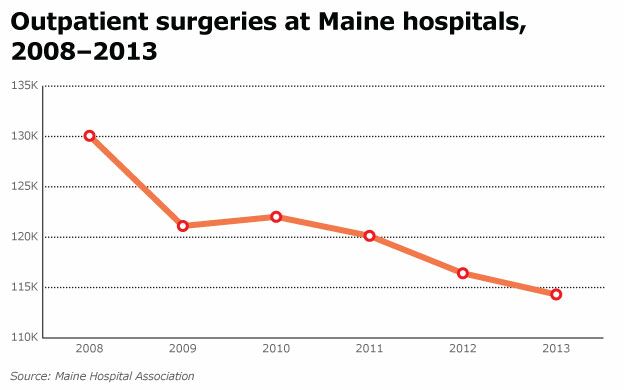
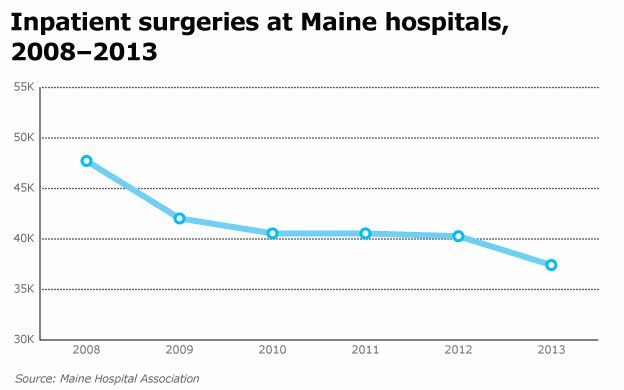
But the No. 1 thing we're seeing that has really jolted our health care system is the decline in 'patient volume.' There are fewer inpatient and outpatient visits and admissions and procedures. That is what is really affecting us.
MB: It's reducing revenues?
SM: Absolutely. I often say, hospitals will really scream about a 10% cut, say, to the Medicaid program in their payments, or the Medicare program … and they should. But when you see drops in volume — meaning patients don't show up — that's a 100% cut, that's 100% revenue that didn't show up. It's not just a little off the top. And that has really jolted the system and is creating unprecedented challenges.
MB: Aren't hospitals driving some of that reduction in volume, by putting greater emphasis on proactive care and doing everything they can to keep people out of the hospital?
SM: Absolutely. That's the ultimate paradox. I mean, what business would do what we do: Encourage doctors to keep people away from you?
But we know, first of all, it's the right thing to do for the patient. Secondly, the system is not affordable. We know that. We know that we're a part of that. It's not lost on us that health care costs are unaffordable and are deterring the growth of Maine's economy — and, more importantly, hurting individuals as they struggle financially.
MB: Isn't a key driver of health care costs emergency room visits for routine care?
SM: Yes. We have very high emergency room use in Maine. It is way above the national average and it's been that way for years. I started looking at the data in the 1990s and that was the case then. It's been a long-time problem. So, we go to work on it. One approach is that some hospitals have adjusted their physician practices' hours, so you have more weekend and evening hours now. We've also had hospitals establish walk-in health care clinics. Brunswick is an example. There's a downtown walk-in clinic. Mid Coast Hospital did that for the very reason of taking pressure off of the emergency room.
MB: What about the focus on keeping people healthy?
SM: Many, many hospitals are doing this. It's labor intensive, but there's a lot of money to be saved and it's good for patients. You try to prevent disease from happening. But once it happens, you manage it. Let's take diabetes, for example. You can manage that on the out-patient basis very well if you make sure the person is taking their blood test, taking whatever [prescription] drug they may be on, eating appropriately, etc. So we have nurses calling people from the hospital, reaching people at their home and asking them how they're doing and whether they've done their 'pin prick.'
MB: But how do you get paid for that? You're providing the service, but it's a service that keeps people from walking through your door and the old payment model of 'fee for service' isn't really designed to cover that kind of proactive service.
SM: Exactly. So there's the paradox. It's great for the patient, great for the business community and it's helping to reduce overall health care costs. But it's hurting us, because under the current system we do not get paid to do those kinds of proactive services.
Right now through the ACA and other initiatives, there are baby steps being taken to change that: Accountable Care Organizations are a prime example. The jury is very much out on those.
In the meantime we're still solidly — I would say at least 85% —in the fee-for-service category and we're slowly changing into this other payment model. We've got one foot in the canoe and one foot on the dock. But here's the problem: That fee-for-service payment system isn't ready to change, in particular at the federal level, where Medicare drives so much of everything in the system. That's why we're seeing those unprecedented changes and financial pressures that we've never seen before.
MB: Even so, many hospitals and various physicians groups are moving in the direction of changing the delivery of care to be more proactive in keeping people healthy, even though the fee-for-service payment model hasn't evolved to keep pace.
SM: Absolutely. They're not holding back. They're not waiting. And what we're seeing is unprecedented losses and that, unfortunately, impacts our work force. We've seen extraordinary cost cutting in Maine. Hospitals have had to do that while their volume is declining and before this payment system changes. So, we're pushing hard at the federal level, in particular, to change that payment system. There are pilot programs going on, but for us, it can't change fast enough. That's the dilemma, and it's a national dilemma. It's happening everywhere.
MB: With Maine being a largely rural state with a good number of smaller hospitals, could you explain how the smaller hospitals are doing in the face of these challenges?
SM: We have 16 critical access hospitals — a federal designation that means they have 25 beds or less. That's 16 of our 37 hospitals, so that's a big chunk of our members. The designation also means they can't keep a patient longer than 96 hours. There are all kinds of other restrictions on them that were established by the federal government in the late 1990s. Now the reward for doing all of that — which effectively prevented those hospitals from doing certain kinds of surgeries and resulted in them sending those patients to Bangor or Portland or wherever — is what's called cost-based reimbursement. While the other hospitals get paid 87 cents on the dollar, or whatever it is right now for Medicare, the critical access hospitals get paid on the basis of their actual costs. That was the reward for doing all those restrictions. It was Congress' way of saying, 'Look, we've got to be careful about preserving access in rural areas.' Without that 'critical access' hospital designation being created in the 1990s, the state of Maine would look very, very different today. It preserved access to health care in rural Maine in big, big ways.
So that's the context.
Now, to answer your question: While that designation has helped, the smaller hospitals are bumping into all of the things we just talked about. But they're smaller, so they have less money, they have less financial reserves and, in a lot of places like Washington and Aroostook counties, they've got declining populations. At the same time they are having to do the kinds of things that the larger hospitals are doing — for example, investing in information technology. That's a huge expense. Another huge expense are the demands on the smaller hospitals to achieve high quality care as well as reduce medical errors. A lot of those demands are labor-intensive and technology-intensive. So the smaller hospitals are particularly stressed in terms of capital needs. As a result, you are seeing many of them knock on the door of the larger health care systems and becoming part of those systems.
MB: In other words, they gain access to deeper pockets?
SM: Yes. Access to capital is a big thing, although it's important to note that Maine Health and Eastern Maine Health and Central Maine Health just don't dole out money. … That being said, we have lots of hospitals that are still independent. We have a lot of hospitals that will be independent for as long as we're around.
MB: What about the larger hospitals, what pressures are they facing now? And what do the larger systems like MaineHealth, Eastern Maine Healthcare and Central Maine Healthcare gain by accepting smaller hospitals into their systems?
SM: I'm going to give an answer that a lot of people won't believe. But it's true. A lot of it is that they see it as their mission, as their greater mission of preserving access in a lot of rural areas. They know they have the expertise; they know they have the resources, even though they're dwindling, and that's what drives a lot of it.
I realize a lot of people will think, 'It's to get their patients' or 'It's to develop a feeder system.' But if people fully understood how things work, those larger systems basically get the smaller hospitals' patients now. I can't think of a single situation where one of the systems went to a hospital and said, 'Hey, we're going to acquire you.' It's the other way around.
The latest example is Franklin [Community Health Network] coming to MaineHealth. Franklin has just done gangbusters on the kinds of things we were talking about: Keeping people healthy, changing their medical staffs' hours, reducing readmissions. But it killed them financially. They put feelers out and said, 'Hey, we think we're not going to be able to make it alone.' They ended up going with MaineHealth. That's just one example of a smaller hospital reaching out to a larger system.
MB: The large systems, what are some of their unique problems and how are they dealing with them?
SM: I don't know if there is anything unique to them. They're dealing with all of the same issues that we've been talking about: They're struggling with declines in volume; the payment system not changing fast enough for them; exploding uncompensated care; all the demands on them for quality. I don't think there's anything unique. The systems themselves, of course, are looking at their own futures and how they can strategically place themselves in that respect.
MB: In Portland, Mercy Hospital completed a major expansion with a new campus at the Fore River site. Soon after, they put themselves on the market, and eventually Eastern Maine Healthcare Systems became their parent. You've got 180 miles between those two hospitals. How does that fit into the notion of a 'system'?
SM: You do realize you are asking me a nuclear question. I represent the Maine Hospital Association, and we have both of those hospitals among our members, as well as members nearby here who aren't very happy about that affiliation.
MB: OK, fair enough. Is there a non-nuclear answer you can give?
SM: I'll say this. The systems themselves, because they are dealing with so much unprecedented change, are at least examining the question 'Are we big enough'? To us in Maine they're big. But in the scheme of things, when we look at what is going on in other states, the systems are becoming regional and national. So you saw what Mercy did, you're exactly right: They put themselves up and said 'We're not making it on our own' and for a while, if you remember, they were being looked at by Steward Health Care System, a Massachusetts for-profit company.
So the systems themselves are looking at whether they're big enough to weather the storm that we're in. They are constantly evaluating that and looking at whether they need to affiliate with others. The Mercy-EMHS affiliation is just one example of how a lot of lines are being erased that we were used to.
MB: You've mentioned there's been a major increase in uncompensated care. Wasn't that supposed to diminish under the ACA because uninsured people would now have health insurance and presumably are now able to pay for their care?
SM: Two things: 1.) We didn't expand Medicaid. In fact, here in Maine, we cut Medicaid enrollment in the last couple of years. So, two things: We didn't expand it and we threw people off the rolls. So part of it is due to that. To be fair, the ACA just really started last year in terms of expanding coverage. And many parts of it have been delayed, as we know. So it's too early to see how many of those who were uninsured are now covered and don't show up as charity care. 2.) Remember the issue of out-of-pocket costs. Even under the ACA, you're going to have a lot of people with modest income coming into the world of the insured but having big out-of-pocket costs. Some of that is going to be bad debt for us. Don't get me wrong: A lot of people do try to pay their bills. But there's no question that a lot of bad debt is showing up right now and will continue.
It's too early to tell what's going on with the ACA. I think the jury is still out, and it will be for a while. When the penalties for not having coverage are so low, there's not a lot of incentive to be covered by insurance. But when those penalties start to increase, who knows?
MB: Medicaid expansion to include roughly 70,000 residents under the state's MaineCare program obviously was a big issue in the last session of the Legislature, with Gov. Paul LePage successfully vetoing three bills that tried to do just that. Why is this important to Maine hospitals?
SM: It's important to know how we even got here. When the Affordable Care Act passed, they looked at two ways of expanding coverage, which was the No. 1 goal of the act. One was to create the Health Exchanges that we all know about and another was a very substantial Medicaid expansion. And all states were going to have to do it.
When the ACA was challenged at the Supreme Court, the court upheld the vast majority of the ACA, but told the federal government, 'You can't mandate to the states that they are going to expand Medicaid and take the federal money that was provided to do so.' So that's how we got here. That was a very significant part of the Supreme Court decision. About half the states have expanded Medicaid and about half haven't. Maine clearly is one of the state's that haven't.
Here's why it's so important to us. The way that much of the ACA is paid for — meaning the subsidies on the Health Exchange and where they got the money to expand Medicaid — was by cutting Medicare. The argument was: 'Hospitals, you're getting all of these newly covered patients and all of this new revenue. You can give up Medicare revenue to help us pay for this.'
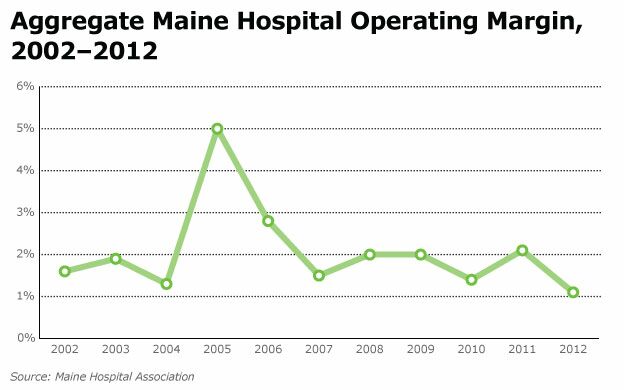
So they took about $155 billion out of Medicare over 10 years, that's nationally. Maine hospitals lost more than $33 million in Medicare cuts in 2013. For us it means about $900 million over 10 years of cuts in Medicare payments in order to pay for the ACA. Approximately two-thirds of our hospitals have negative operating margins. That's an all-time high.
So, our view is: We're paying for all of this. By not expanding Medicaid, we get the double-whammy. We get the Medicare cuts for sure and we don't get the benefits of new Medicaid revenue because, here in Maine, we didn't expand that program. That's our No. 1 issue.
The other thing, which thankfully was resolved in the least session, was the nine-year problem with our Medicaid debt. Everyone agreed the state needed to pay its share of that debt. But if you remember, one of the things the Maine Hospital Association said in support of the state paying roughly $170 million is that it would trigger the federal government paying the remaining $330 million of the overall $500 million debt. We said that money could be used here in Maine sustaining jobs, creating jobs and flowing into the state's economy instead of sitting down in Washington, D.C.
From the perspective of Maine hospitals, the same principle would apply if Medicaid was expanded, there would be federal money coming in.
MB: How much?
SM: Ironically, about $300 million to $350 million in new money annually; that's once it's fully up and running in 2016 or 2017. It takes a while to enroll folks.
At the same time, we acknowledge the governor's point: There is a state cost to this. A lot of people who keep saying 'It's free federal money' need to be very careful. It's not. There will be a state cost to this and we acknowledge that, and we have done so from the very beginning. We understand that concern.
But for us the math is just too compelling. For very little state money, 5% initially to 10% in 2019, when the federal government's share of the Medicaid expansion goes down to 90%, that's still a 90% match from the federal government! If you see anything like that as a federal match for a highway bond, everybody breaks out champagne and uncorks it in celebration.
We do acknowledge there's a hit to the state; how much depends on the number of people covered by the Medicaid expansion. But overall I just don't know how you can ignore a 90% match from the federal government. That's where we are. It really gets back to the fundamental fact that we are already paying for it through the Medicare cuts. So we're asking, 'Can we please get some of that money back? We're losing it under Medicare, can we get it back under Medicaid? That was the plan. Can we stick with the plan?' I would also add, with the explosion of uncompensated care, it sure would help.
MB: Setting aside problems and challenges, what are some of the good things happening at Maine hospitals?
SM: This is a field in which there is a dearth of good news. But one important success story is that for several years now — and there have been several different national groups doing the measurements, not just one — Maine hospitals cumulatively have been ranked No. 1 in quality of care. It's a testament to the hospitals' commitment to it. As is case with all organizations: It starts at the top. I give my CEOs a great deal of credit for driving this agenda, but it really comes down to all of the care-givers. It's a great testament to our 37 hospitals that are pursuing safety and quality of care every day and they're literally the best in the nation, and have been for a few years now.
MB: Is there any last message you'd want to convey to the Mainebiz audience, C-level executives, owners and corporate decision-makers?
SM: To really get at the root causes of affordability problems, employers have a major role to play. We can help them, and they can help us. That's a ready-made partnership right there. Here's an example: Bath Iron Works gives incentives to their employees to go to a health-screening clinic. And they'll give them a little reward, a gas card or whatever it might be, to get them to go to a screening to get their blood pressure done or their cholesterol level checked.
So talk about a great partnership: The hospitals and physician practices are doing all kinds of things in that regard, but when employers join in that effort it has a huge benefit.
Read more
Norwegian health officials visit Maine hospital
Anthem, EMHS partner for new health program
Mercy back in the black, credits EMHS merger
6 Maine hospitals face penalties for complications
MaineHealth gets $9.2M for cutting costs
Maine Medical Center opens 24/7 pharmacy
Pen Bay, Waldo County Healthcare to partner under new parent company











Comments